Stroke patients in South Korea will be the beneficiaries of a landmark series of joint simulation workshops to optimise the prehospital pathway and reduce treatment delays.

In an auditorium at Chungbuk National University Hospital on Thursday 18 November, a woman falls and rolls onto her side where she lies, groaning softly. A friend rushes to her side. An ambulance is summoned and after six minutes help arrives, and the patient is strapped to a stretcher and deposited in a location a few metres away from where she fell.
There are now several clues that this is no ordinary emergency. The patient, her friend and the trio who come to their aid are all wearing the striking orange and black uniforms of the South Korea fire service, and so are about two dozen others in the room who are manning mobile desks and taking notes as the action unfolds.
Given that everyone clad in orange knows the inside of an ambulance like the back of their hand, it takes no effort to imagine they’re barrelling along the bustling streets of Cheongju, the capital of SouthKorea’s North Chungcheong Province, or that a raised stage below a giant screen with a close-up image of the gantry of a CT scanner represents their destination, a hospital’s emergency room.
What you are witnessing is only the second ever joint simulation workshop involving a stroke-ready hospital and a 119 team from South Korea’s fire brigade and ambulance service.
Operated by the National Emergency Management Agency (NEMA), ambulance services in South Korea are professional, well-organised and provided free of charge. But as is true of emergency services in most countries around the world a lack of co-ordination between ambulances and hospitals negatively impacts onset-to-treatment times and ultimately patient outcomes in medical emergencies such as stroke.
It is for this reason that the Angels Initiative team in South Korea and four participating hospitals petitioned NEMA to greenlight a landmark series of joint simulation workshops to optimise the prehospital pathway for stroke patients.

The first step is always the hardest, reflects Sungsin Park, Angels Programme Manager for South Korea, for whom the series of joint EMS simulations conducted during 2021 spells the start of an extended campaign to reduce onset-to-door and door-to-treatment times.
Simulation training is a valuable tool for stroke pathway optimisation. It reduces treatment delays and improves performance by identifying bottlenecks in participating hospitals, lays the foundation for a mutually agreed multidisciplinary action plan for implementing solutions, and cultivates a quality mindset.
But however diligent hospital and prehospital teams are about streamlining their respective pathways, it is at the interface between hospital and EMS where precious minutes can be saved, with far-reaching consequences for stroke patients.
The co-operation of a government agency in South Korea with hospitals and the Angels Initiative was a groundbreaking development and the result of extensive planning and communication. The first joint simulation took place in Changwon Gyeongnam Province, at Yonsei S Hospital, one of the hospital that specializes in stroke care, on 26 July. Its success paved the way for three more simulations – at Chungbuk National University Hospital in Cheongju in North Chungcheong Province, Kyungpook National University Hospital in the Daegu Metropolitan City, and at Kangwon National University Hospital in Chuncheon in Gangwon Province.
For Sungsin and his team, the project marked a steep but ultimately satisfying learning curve. Scenarios were developed at the Stroke Simulation Centre in Brno in the Czech Republic and adapted to local conditions. Participants were thoroughly briefed on training goals, their assigned roles, and patient information. And to implement corrective action agreed during the debriefing, simulations were repeated.
Angels team member and simulation coordinator, JuWan Kim, had signed up for training in video recording and editing, to produce clips that are an important aid in reviewing performance and prompting team discussions. So well produced were the clips done by JuWan, that they will now become field manuals to support training within the regional prehospital system.
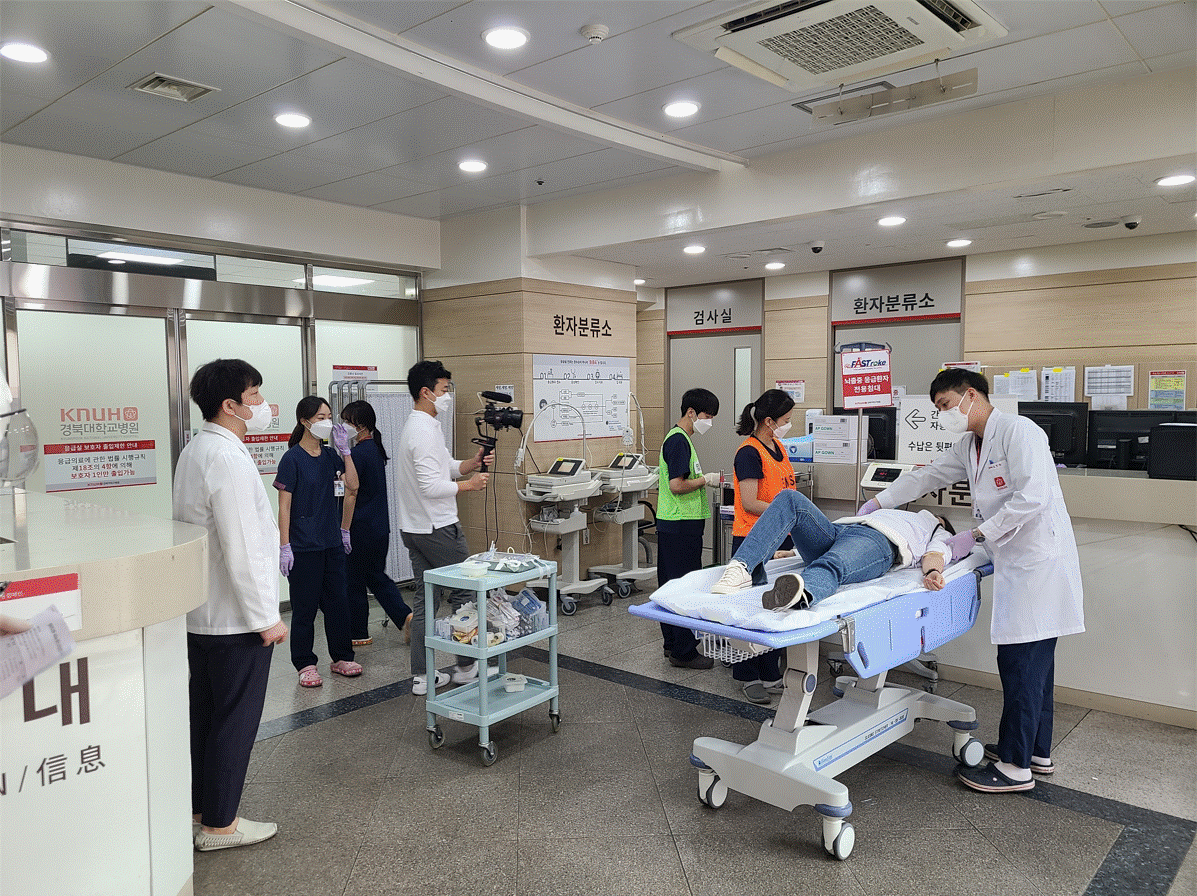
The simulation at Kyungpook National University Hospital commences in an ambulance, where a 119 officer works swiftly to assess the patient while taking information from a family member. The hospital is pre-notified and when the ambulance reaches its destination, a nurse and ER physician meet them at the entrance. The patient is conveyed directly to the CT imaging room, before being wheeled to the emergency department for treatment.
“So many doors,” the stroke physician remarked when reviewing the footage. It is one of the literal barriers this hospital will address in their action plan.
The simulations showed up several opportunities for improvement, Sungsin says. “The pre-notifications aren’t properly utilised. Physicians and nurses repeat the same neurology assessments. Too much time was spent on obtaining patient consent and as a team, they did not share all the relevant information with each other. Processes vary from hospital to hospital, indicating a need to standardise protocols.”
One thing however, is remarkably consistent across all four simulation videos – in every instance, a sense of mission is in the air, as participants give their all in the task. Further training can help shape the path and offer more stroke patients a second chance in life, but the emotional commitment from the teams on both sides of these hospital doors, is something you cannot simulate.