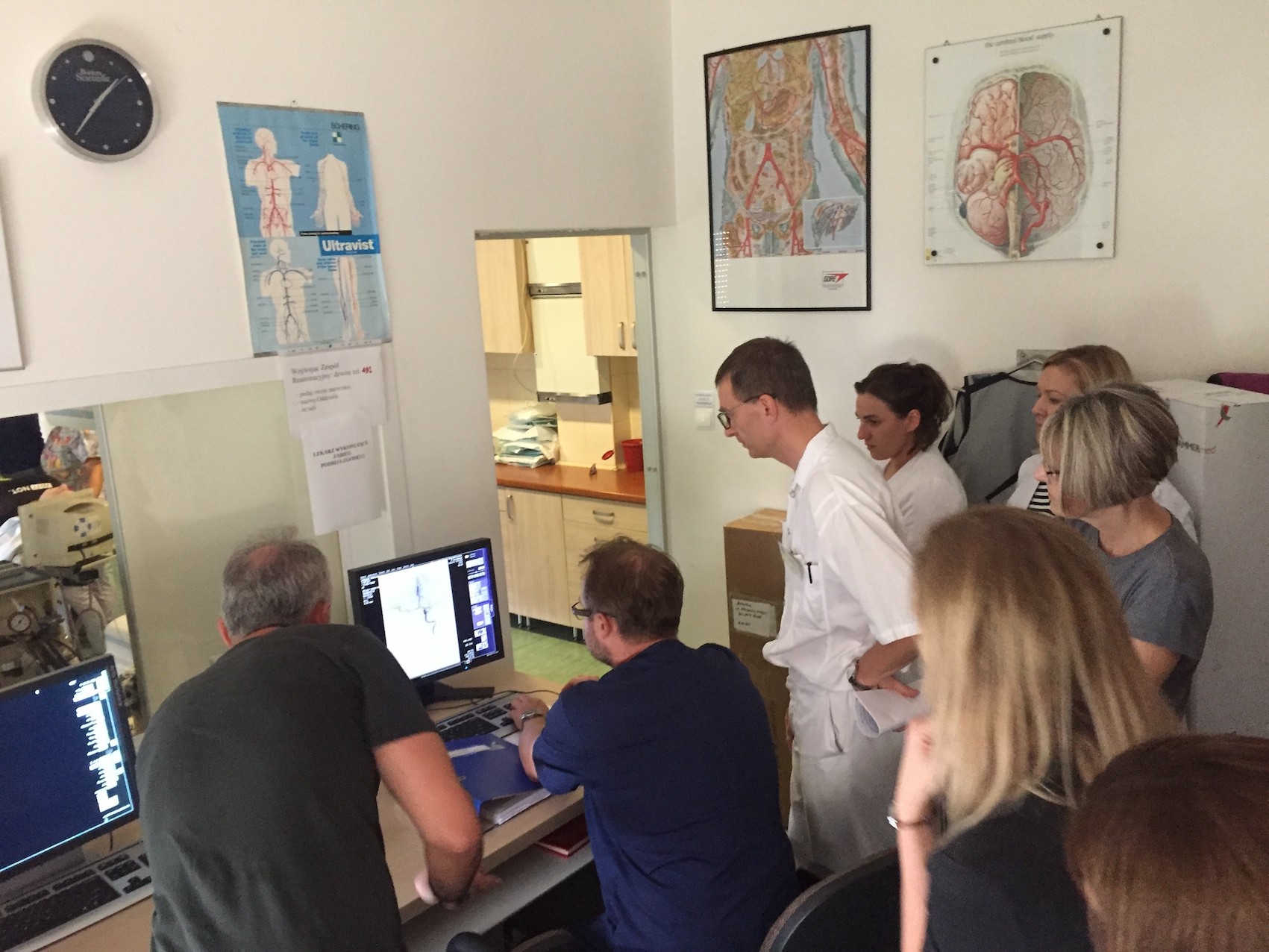
A pathway simulation at a high-functioning Poland hospital was a learning opportunity for new doctors as well as a neighbouring hospital, and a reminder that the duty of being good is to be better.

If you want to know how a regional hospital in Olsztyn in northern Poland achieves a door-to-needle time of around 10 minutes, you’ll find the answer outside the door. As the ambulance pulls up at the entrance having notified the hospital a stroke patient is on the way, is there a neurologist waiting inside the doorway? No, there isn’t.
That’s because the young stroke doctor on call has already jumped inside the ambulance, determined that not a second should go to waste in the bid to save the patient.
For this doctor nothing else matters in that moment, says Angels consultant Agnieszka Tymecka-Woszczerowicz who after four years in the field is still moved by a wholehearted expression of dedication. “He treats every single patient as if they were his family.”
The desire to provide the best possible treatment to every stroke patient has lead to impressive treatment times for Voivodeship Specialist Hospital, a comprehensive centre in Olsztyn and the leading medical institution in the region of Warmia and Mazury, and was the motivation behind an impromptu pathway simulation with multiple goals that took place in Olsztyn a couple of summers ago.
Open the door
Voivodeship Specialist Hospital in Olsztyn is one of 20 hospitals in Poland with the capacity to treat stroke patients with mechanical thrombectomy. Although well short of the estimated 38 comprehensive centres needed to serve a population of over 38 million, this number
is testimony to the leadership of Spirit of Excellence award-winner Professor Anna Członkowska who in 2019 announced to a meeting of around 300 neurologists: “Remember, when Angels knock on the door, open it.”
In the four years since, the Angels team in Poland has adapted its programme to the country’s changing needs, which has included facilitating regional training for managing the thrombectomy pathway, and workshops and webinars about interpreting CT Angiography scans to diagnose large vessel occlusion.
Simulation training, a key tool for speeding up time to treatment with thrombolysis, typically focuses on the path from door-to-needle. Pathway simulation that covers the extra mile to mechanical thrombectomy is less often on the training agenda, but the team at Voivodeship Specialist Hospital in Olsztyn were determined to not only test their door-to-needle performance against the clock, but also to identify barriers in the pathway from door to groin.
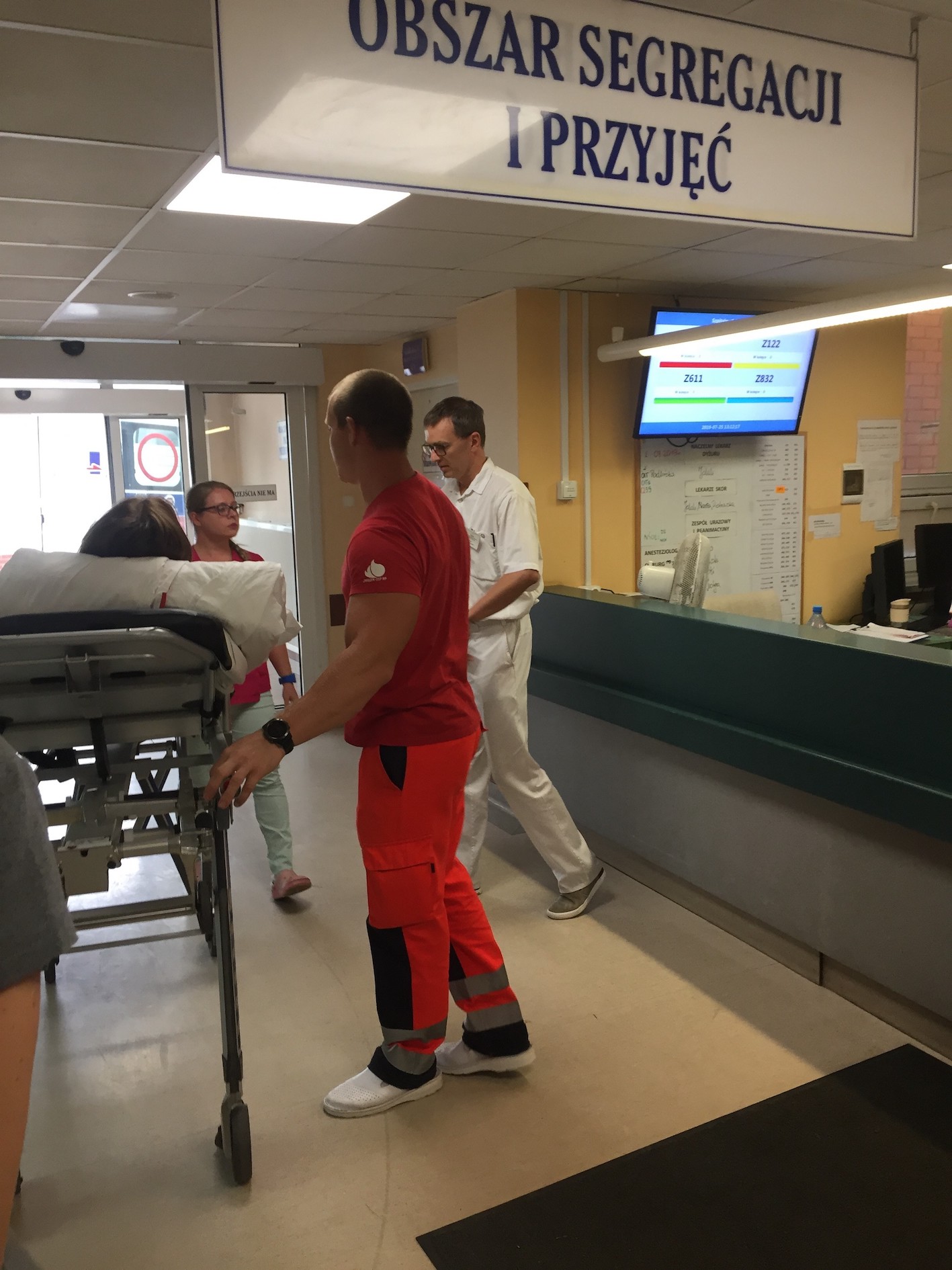
Catch the moment
Voivodeship Specialist Hospital had not been on Agnieszka’s list when she traveled to the region to conduct simulation training at several primary stroke centres in and around Olsztyn. But she had to extend her stay after the head of the stroke unit at this leading hospital declared that his more experienced team could likewise benefit from reviewing its own performance.
It was a case, Agnieszka reflects, of “catching the moment”.
The hospital was already committed to treating patients with thrombolysis at CT, as evidenced by a door-to-needle time that was typically around the 10-minute mark. But they had recently been joined by several new doctors and in addition saw an opportunity to be of service to their neighbour, the Clinical University Hospital in Olsztyn, that had a new stroke unit and where a pathway had to be created from scratch. The University Hospital would later go on to win three consecutive diamond ESO Angels Awards.
Besides finalising the clinical scenarios and inviting the neighbours, preparations were made for creating an educational video to be used outside the hospital to train more doctors in future. In addition to its other simulation achievements this created the opportunity for greater visibility at a national level.
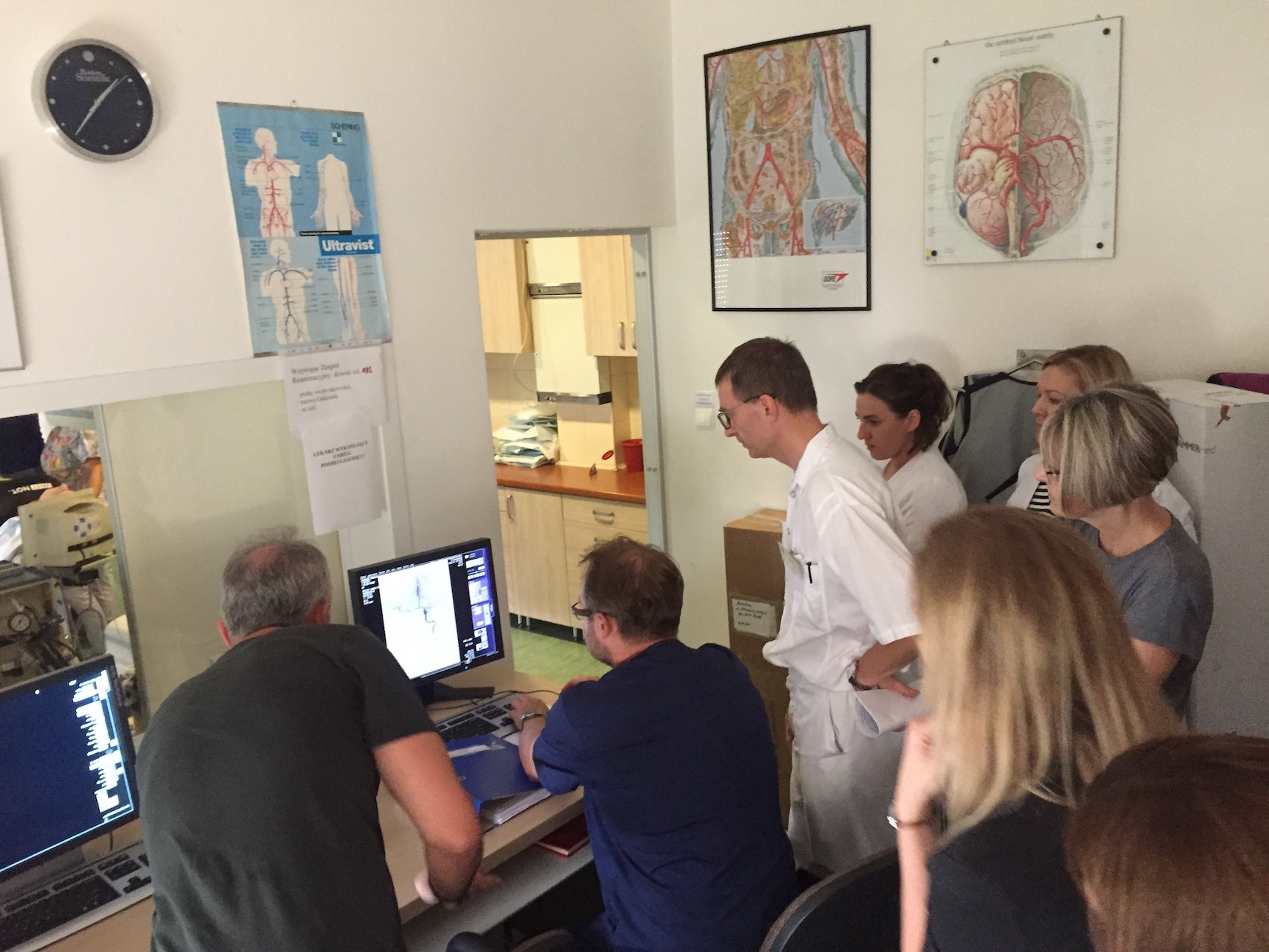
Go the extra mile
The “patient” arrived at the hospital three minutes after ambulance prenotification alerted the stroke team and there was, unsurprisingly, no delay between arrival and first medical contact. An NIHSS screen was performed one minute later and after two minutes Code Stroke was activated. Four minutes in, a blood sample was sent to the laboratory for analysis. At six-and-a-half minutes, the patient glided into the CT scanner. The decision-making clinician analysed the results and reached a therapauetic decision in 3 minutes and 30 seconds.
Treatment commenced 11 minutes after the patient reached the hospital door, and an angioCT scan took place at the same time. Then the simulation proceeded to the angio suite; in a real-life situation, the catheter would pierce the skin at the groin in under 40 minutes.
It was an impressive performance, but because good can always get better, it was agreed in the debriefing that the hospital would arrange to acquire a point-of-care INR device to remove the need to test blood samples away from the patient.
The simulation was memorable for another, unplanned reason.
At two points during the process, the action was paused for the 20-odd doctors present to receive an impromptu lesson in interpreting CT and angioCT results. Though not in the game plan, it had seemed as good a time as any for some advanced training that would help the doctors in the room sharpen their decision-making skills.
When lives are at stake, it makes sense to catch the moment.