
An arrow that targets recovery
An early-morning swim sparked a bright idea for staff of the stroke unit at the Regional University Hospital of Málaga. A red arrow indicating the location of the change room triggered a train of thought that lead to the Arrow Project, an intervention to remove variability in the post- acute phase of stroke.
The fact is that not all stroke patients have access to specialised stroke units where post-acute protocols are strictly implemented and supervised. Many stroke patients are cared for on wards in spoke hospitals where the protocols are not entrenched in routine, a situation that is exacerbated by the rotation of nursing teams.
Proyecto Flecha uses arrows placed at the top of each patient’s bed to help doctors, nurses, nursing assistants and even porters easily identify the type of stroke and side affected, and via a QR code access details of the treatment protocols for each day, such as regular checks for dysphagia, glycaemia and fever.
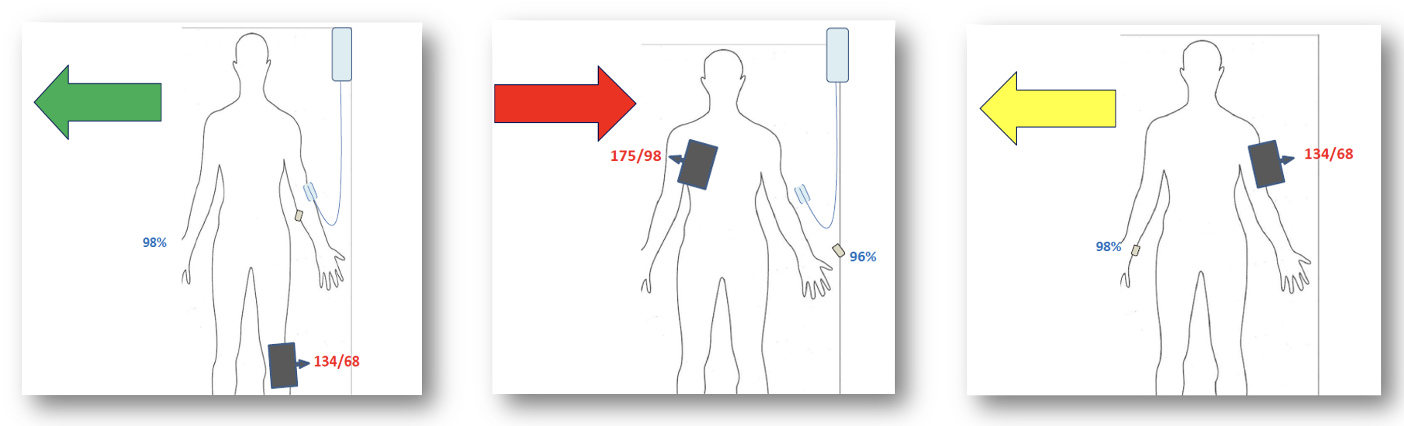
The first visual cue is the colour of the arrow – red for haemorrhagic stroke, yellow for ischaemic stroke and green for subarachnoid haemorrhage. The second cue is the direction of the arrow that indicates the affected side so even staff members who have just come on duty will know instantly on which side to place the blood pressure cuff and intravenous line, where to attach the pulse oximeter for measuring blood oxygen levels, how to approach mobilising the patient and which side is optimal for patients whose communication abilities are impaired.
It seems a lot to expect from a simple shape with a wedge at one end and a triangle at the other, but the Proyecta Flecha arrow has shown itself to be a powerful weapon in post-acute care and more than equal to its task.
Outside of public swimming pools, popular culture has invested the arrow with symbolic meaning that includes reaching one’s goals and achieving targets. It also represents protection from harm, something that Proyecta Flecha delivers to stroke patients every day.
***
A stroke phone that works
It is just a phone, like you and I carry. But when it is used to save a life, it becomes a stroke phone.
This was the experience of the stroke team at Sumy Central City Clinical Hospital in Ukraine during a simulation to improve communication between the neurology department and ambulance service and bring the hospital closer to its goal of providing the best stroke treatment in the region.
It takes just a few simple steps to optimise the patient pathway and ensure everything is in place for swift decision-making so treatment can start without delay. A neurologist meets the patient at the door, there’s a clear path to the CT room and all the relevant information is collected while the CT is being performed. But what sets this chain of events in motion is a very important call to a very important phone.
A stroke phone that connects the EMS directly with the neurology department is the most expeditious form of prenotification, alerting the stroke team that a stroke patient is on their way. Sumy Central was one of few hospitals that had agreed to this intervention – but between having a stroke phone and using it, there existed an implementation gap.
It’s important to check the phone works, says Angels consultant Maria Sheverdina who conducted the simulation in Sumy in northeastern Ukraine. And by this she doesn’t only mean checking that the device is charged and the connection stable.
"A stroke phone is not just a device, it’s a process,” Maria explains. And making the process operational was the chief focus of the simulation.
The teams from both EMS and Sumy Central had brought their A game and the exercise proceeded smoothly right up to the moment when the EMS physician placed a call directly to the stroke neurologist and there was a rapid exchange of information about the case. Then the pathway shifted up a gear.
In the debriefing that followed the simulation, several opportunities for improvement were proposed and discussed, but the stroke phone had earned its place in the Sumy Central pathway and it would only be a matter of time before the hospital earned its first Angels ESO diamond award.
With a commitment on both sides to keep the phone in working order – both the process and the device – the Sumy Central stroke phone became the first link in a life- saving chain. For more than one future patient, it will be the most important call ever made.
***

A badge for the best
If you pay a visit to the Cerebral Vascular Unit (CVU) at Hospital de São José in Central Lisbon, you may notice on the lapels of some of its personnel a small green badge that carries a lot of weight.
At the top of the badge is the phrase, “give life a chance”, which is the motto and mission of the Angels Initiative. Below it, are the words “time is brain”, along with a reminder that one minute’s delay costs the acute stroke patient 1,900,000 neurons. Then come the words that tell you something important about the wearer of the badge: “Holder of best needle time of the month”.
Ricardo Braga, a stroke nurse at the unit since 2006, has frequently worn this badge with pride. He explains how it works: “The badges were created to recognise the team with the best door-to-needle time each month. The treatment times for all patients who undergo thrombolysis at our hospital are noted on a poster that is displayed in the locale where the daily multi-disciplinary meeting is held. At the end of every month, the names of the team with the shortest times are extracted from this information, and announced by the unit co-ordinator. Teams are proud to wear the badge and try not to lose it to their colleagues the following month.”
At first badges were only awarded to the doctors and nurses involved in thrombolysis, but now there are also badges for the interventional neuroradiologist and angio nurse with the month’s best door-to-groin time.

The badge has created a spirit of friendly competition, Ricardo says. It stimulates record-keeping and analysis of treatment times and has helped keep the focus on the importance of rapid treatment of acute stroke through an ongoing performance challenge that ultimately benefits the patients the unit cares for. And that is what the badge is ultimately about – “the feeling that we can make a difference and that through our best efforts a significant percentage of patients return to lives very similar to the those they enjoyed before the event”.
And that is what the badge is ultimately about – “the feeling that we can make a difference and that through our best efforts a significant percentage of patients return to lives very similar to the those they enjoyed before the event”.
***

The call to arms
A nurse at Avezzano Hospital in Italy’s Abruzzo region drew attention to a deceptively trivial problem during a consultant’s visit. When patients arrived at the hospital fully clothed, the nurse explained, treatment was delayed by 10 minutes or more while clothing was removed from the patient’s upper body to insert the cannula for intravenous therapy. Precious time could be saved if patients were delivered to the CT room with their arms exposed – but how could they recruit the support of emergency medical services to clear this hurdle?
The answer was three words: a braccio pronto (in English the meaning is “arm ready”). Stickers bearing these words were installed inside the EMS vehicles as a reminder to ensure stroke patients arrived at the hospital ready for treatment to commence without delay.
A simple logo was designed to convey the message with as much clarity and impact as possible, and the words “a braccio pronto” soon came to stand for faster access to a life-altering intervention as more patients were being brought to the hospital with bare arms ready for treatment.



