This time of pandemic has forced us to make many adjustments. As there are no official guidelines to follow, it is sometimes difficult to know exactly which changes the correct ones are.

Whether your country has already been affected by COVID-19 or is still bracing for tougher times, we all must take a closer look at our stroke pathway and consider all the new variables we are facing.
As with optimizing a stroke pathway during “normal” times, there is no silver bullet solution here. It needs to be customized to your local situation and resource capacity, among many other things. But unlike optimizing stroke pathways, there is no official guideline to go by nor do we have the time to wait for it. It is up to us to figure this out ourselves and the best way to do this is by learning from each other.
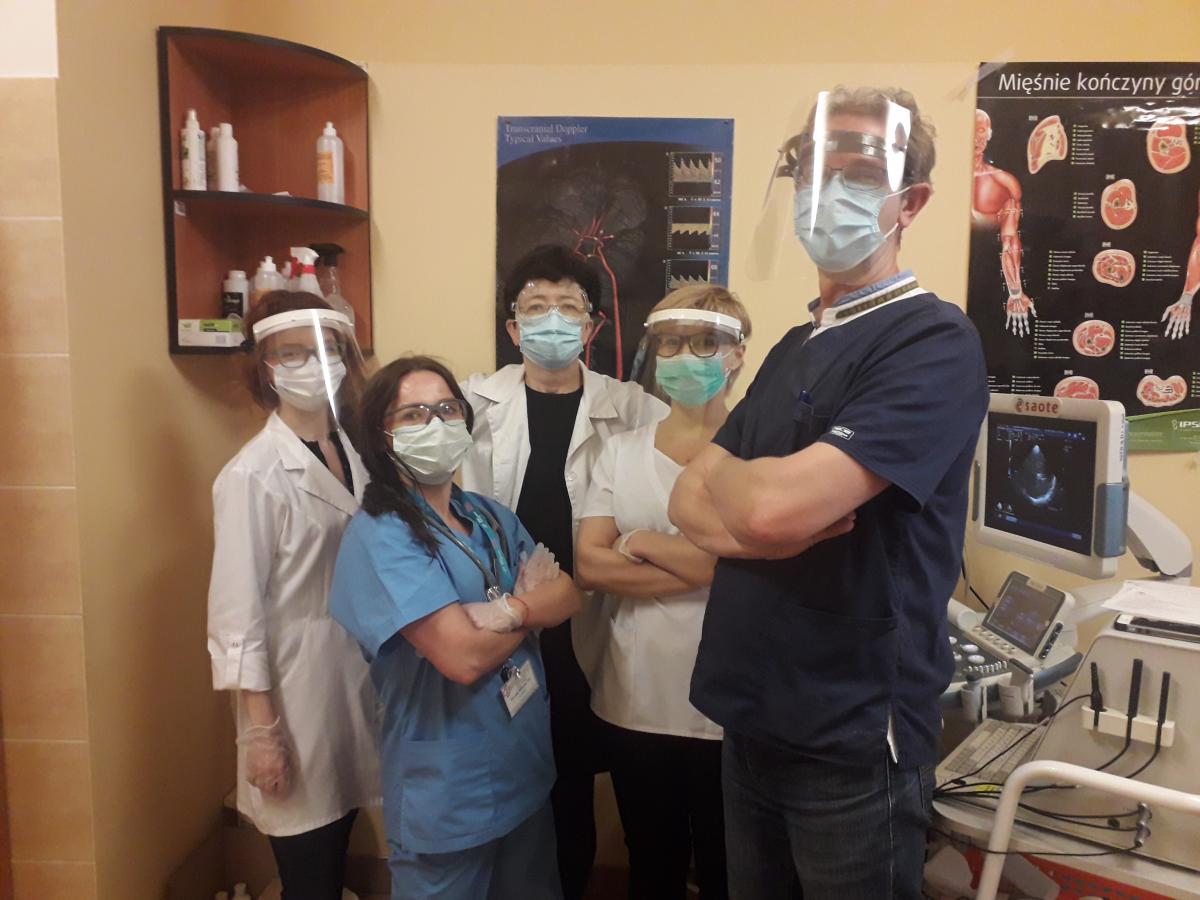
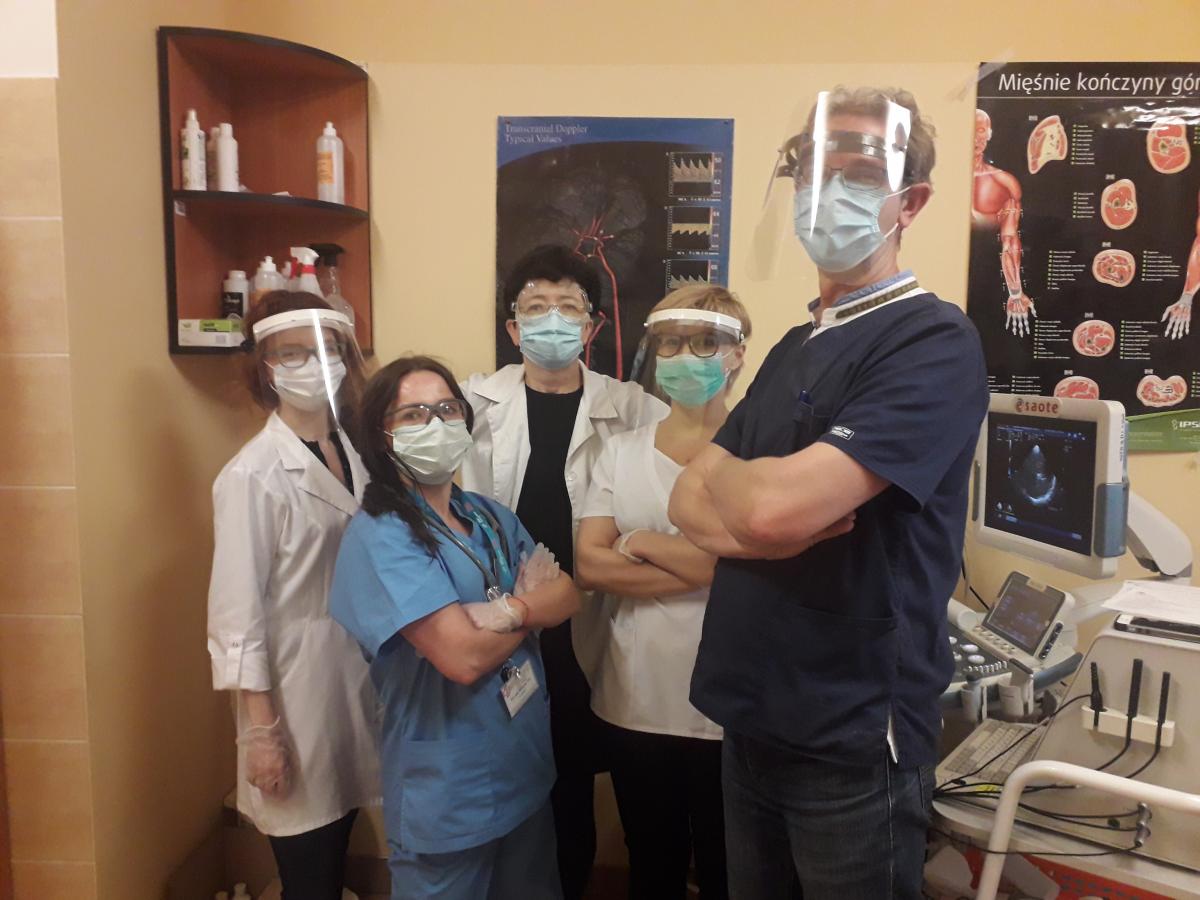
We recently sat down with Piotr Luchowski MD, PhD and Joanna Wojczal MD, PhD who were kind enough to share about the changes in the stroke pathway of Independent Clinical Hospital no 4 in Lublin, Poland, during this time of pandemic. At the time of writing, Poland had the 35th highest total COVID-19 cases in the world with around 22,000 reported cases1.
HOW DOES ADMISSION OF A PATIENT WITH SUSPECTED STROKE AND SIMULTANEOUS SUSPECTED OR DIAGNOSED SARS-COV-2 INFECTION LOOK LIKE IN THE UNIVERSITY HOSPITAL IN LUBLIN?
The patient enters directly from the ambulance driveway to the ED room dedicated for patients with suspected or confirmed COVID-19 infection (red zone). Patients with unclear COVID-19 history due to speech problems or unconsciousness are also admitted to the red zone ED. An Emergency Department Neurologist then examines them, orders the necessary diagnostic tests and consultations, as well as a nasopharyngeal swab test for COVID-19. The ED neurologist with an ED staff member then transports the patient to a CT room, also located in the red zone. Head CT and lung CT scans without contrast are performed for each patient with suspected stroke and simultaneous suspected SARS-CoV-2 infection. The examination is performed by a radiologist and radiological technician. A contrast for angio CT in red zone is administered by a trained ED employee. The treatment decision is made by the strokeologist after telephone/in person consultation with the radiologist.
WHAT KIND OF PERSONAL PROTECTION EQUIPMENT (PPE) IS BEING USED?
Before the first contact with the patient, both ED neurologist and strokeologist use: disposable clothes with long sleeves (disposable surgical gown), disposable gloves with an elongated cuff (at least two pairs - internal and external), goggles or face shields, neck protectors, a hair cap and a face mask with FFP2 or FFP3 filters that adhere well, ultimately a surgical mask. Paper and non-woven masks are not allowed.
WHAT IS THE PROCEDURE WHEN THE PATIENT IS NOT QUALIFIED FOR REPERFUSION THERAPY?
The patient is transported from the CT room to the ED Observation and Isolation Unit. It is strongly recommended to repeat the test (24 hours after the first one) for SARS-CoV-2 infection in the ED Observation and Isolation Unit (so-called confirmation test).
If the result of the confirmation test is negative, the patient is referred to the Stroke Department of the Neurology Clinic for further treatment of stroke. If the result of the test confirms the infection, and the patient's condition allows them to be transported to an infectious hospital, such patient should be transferred after prior telephonic agreement. If the patient's condition does not allow for transportation, the patient is transferred to the Intensive Care Unit in the red zone or remains a patient of the Observation and Isolation Unit.
The neurologist is obliged to consult the patient daily. The consulting neurologist uses PPE provided by the department that is hospitalizing the patient before contacting the patient.
WHAT DOES A PATHWAY LOOK LIKE IF THE PATIENT IS QUALIFIED FOR THROMBOLYTIC TREATMENT?
Strokeologist starts treatment already in the CT room in the red zone (if possible). A stroke bag including the medicine needed and the infusion pump to administer it is located in the red zone ED treatment room. Continuation of the infusion takes place in the ED Observation and Isolation Unit. The Strokeologist is present during the drug administration to monitor the patient's clinical condition.
It is strongly recommended to repeat the test for SARS-CoV-2 infection in the ED Observation and Isolation Unit (confirmation test). In case of a result confirming SARS-CoV-2 infection, transfer to an infectious hospital may occur no sooner than after a CT scan of the head (performed 22-48 hours after thrombolytic treatment).
WHAT IS THE PATHWAY IF THE PATIENT IS QUALIFIED FOR MECHANICAL THROMBECTOMY TREATMENT?
After the CT scan, the patient is transported to the Surgical Room in the red zone of the Department of Interventional Radiology and Neuroradiology, where the procedure is performed. This Surgical Room has been separated from the hospital structure only for performing procedures in patients with suspected infection or SARS-CoV-2 infection, it is equipped with locks for changing and decontamination, and the patient can be also transported from the outside, bypassing hospital corridors. Everyone participating in the procedure (anesthesiologist, anaesthesiological nurse, interventional radiologist, strokeologist, interventional nurses, radiologist technician) is obliged to use PPE. The anaesthesiologist, anaesthesiology nurse, and radiologic team must additionally use FFP2 / FFP3 masks.
After the procedure, the patient is transported to the ED Observation and Isolation Unit or Intensive Care Unit in the red zone. It is recommended that a second SARS-CoV-2 test be performed 24 hours after the first one. If the results of the SARS-CoV-2 test are negative, the patient is transferred to the Stroke Department of the Neurology Clinic.
In the case of a test result confirming SARS-CoV-2 infection, and the patient's health condition allows him to be transported to an infectious hospital, we pass on the patient after prior contact and telephone agreement. Transmission may occur not earlier than after a CT scan of the head (performed 10-48 hours after endovascular treatment).
WHAT IS THE PROCEDURE FOR A PATIENT QUALIFIED FOR BOTH THROMBOLYSIS AND AFTER MECHANICAL THROMBECTOMY?
The strokeologists starts treatment already in the CT room (if possible). The Stroke bag including the infusion pump is located in the red zone ED treatment room. Continuation of the infusion takes place in the Surgical Room in the red zone in the Department of Interventional Radiology and Neuroradiology, where the patient is transported directly from the CT room.
ARE THERE ANY CHANGES REGARDING THE ORGANIZATION OF THE MEDICAL PERSONNEL WORK SYSTEM IN THE STROKE UNIT DURING THE PANDEMY?
In the Stroke Unit, employees are divided into two teams working alternately. Each team works an average of 2 days on a dual basis, after which they rest for 2 days. Such a system was introduced so that if, despite the protective system, there was a patient infected with SARS-CoV-2 virus, only one team (half of the team) goes for quarantine. This will avoid closing the stroke unit due to lack of staff.
ARE THERE ANY CHANGES IN THE DURATION OF PATIENTS' HOSPITALIZATION IN THE STROKE UNIT IN THE CURRENT SITUATION?
Stroke patients, if their condition allows, are not hospitalized currently for more than 7 days as recommended by the National Health Fund. They are discharged after full diagnosis is performed, usually within 5-6 days. We manage to transfer some patients to Rehabilitation Departments. However, the biggest problem we are facing currently is with those patients who have large neurological deficits and are bedridden. Care and Treatment Centers do not currently want to admit new patients, so if the family is unable to provide care, the hospitalization needs to be extended.
1 https://www.worldometers.info/coronavirus/country/poland/. Retrieved on 28 May 2020.