In June 2016, during one of our Angels initial meetings, Professor Igor Voznyuk took a strong interest in the use of the Body Interact software for conducting trainings in the St. Petersburg Research Institute of Emergency Care – a big, multi-functional hospital as well as a research and educational institute for medical universities. Within months, he started doing simulations using Body Interact with his team.

It was only natural that, upon hearing about it, Professor Voznyuk became interested in a Stroke Simulation Center managed by Dr. Robert Mikulik and his team in Brno, where they train using real case simulations. He visited the Simulation Center in November 2017 and gained further inspiration on how to better stroke care in his network.
It was never going to be easy, but Professor Voznyuk knew that setting up an educational-based simulation center would dramatically improve the training of stroke teams in his region.
The challenge was then to convince the right people that this simulation center idea is a worthwhile investment to improve stroke care at a regional and, eventually, national level.
The concept itself was further adapted from the Brno blue print to local reality and needs.

Eventually, on the first of June 2018, the course was launched during a conference dedicated to emergency care in St. Petersburg, where he hosted a simulation-themed symposium.
The plan is to offer the simulation-based training course at the St. Petersburg Research Institute of Emergency Care, where he would be able to emulate a hospital environment better and conduct trainings on a regular basis.
The simulation course is divided into five phases:
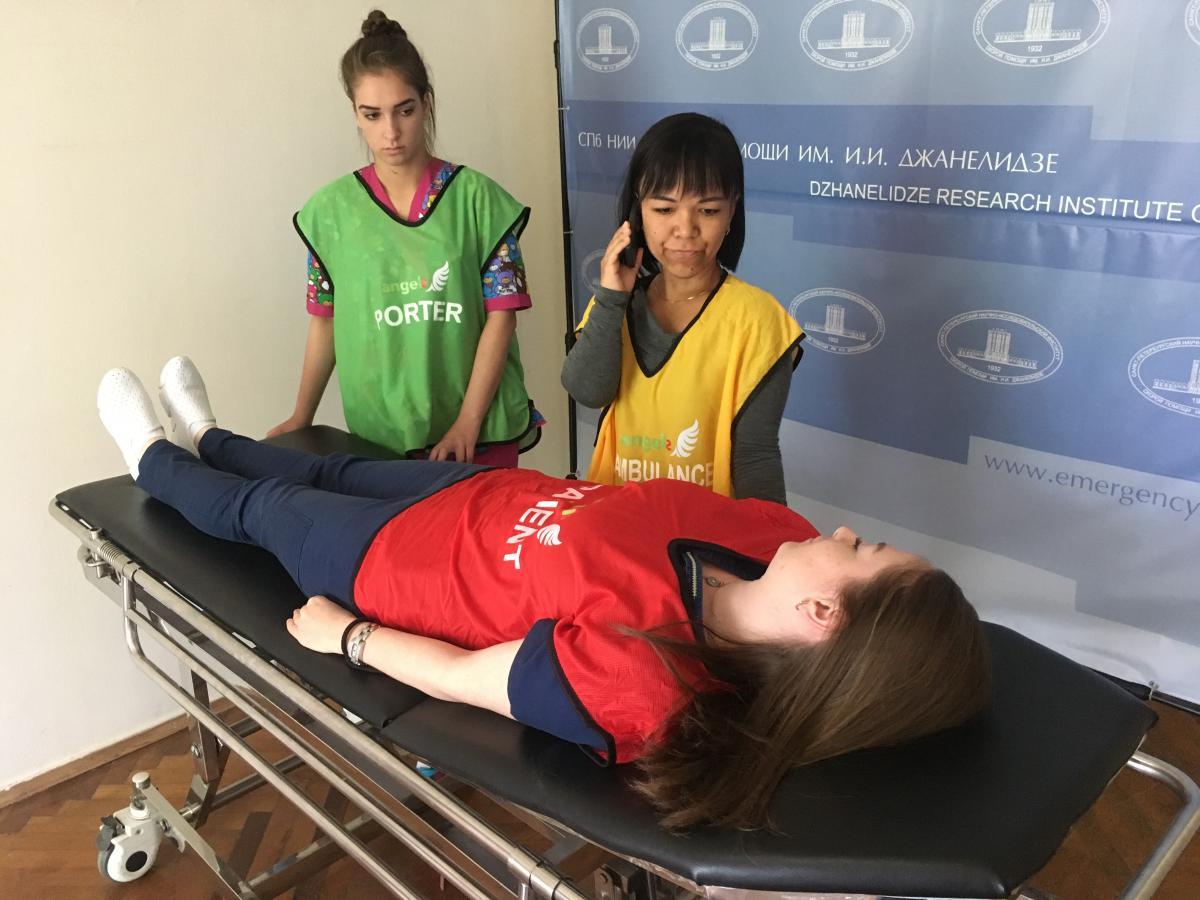
- Pre-Hospital phase with a full interview and assessment of the dummy patient by ambulance, using the FAST protocol;
- Transferring of data from the ambulance to the hospital: phone call and then face-to-face transfer of patient to the Stroke Team at the hospital;
- In-Hospital phase from door to treatment;
- Feedback from observers and experts board;
- Q&A session
Those receiving the trainings consisted of stroke unit staff members from different hospitals and ambulance staffs from different ambulance services, who were divided into 4 training groups which included a dummy patient (and a relative, if the scenario called for it), an ambulance crew, a porter, a neurologist, a nurse, as well as observers and juries armed with a checklist developed by Professor Voznyuk for feedback.
At the start, only the dummy patient and his relative knows the exact scenario, based on a case from Body Interact. The task of the ambulance crew is to collect all applicable information, diagnose the patient, and pre-notify the stroke team using a stroke phone.
The patient is then transferred on a real trolley to the “hospital” where the neurologist and nurse are waiting. Patient’s transfer from ambulance to neurologist and initial interview and assessment is followed by Body Interact case start, which is displayed on a big screen and operated by an Angels consultant. The task of the stroke team is simple – to diagnose and treat the patient.

Once the simulation is done, a jury of four chiefs from different stroke units who have been observing the process will share their feedback based on the notes and scoring system that is part of the observer’s checklist; touching upon aspects such as cooperation and communication between team members and with patient, time loss issues and protocol compliance. This would then be followed by a Q&A session to ensure full understanding among all parties involved.
The simulation courses are currently set to take place once every three months, inviting every advanced neurologist from the region’s stroke units. But as with all great visionaries, Professor Voznyuk and his team have set their eyes on to bigger things; aiming to increase the training frequency to a monthly basis and involving regions other than their own. They are also looking into formalizing this course as an elective module for the national certification of neurologists, so that participants can claim points creditable to their neurologist certification (which per local regulation must be renewed every five years).
In considering to set up a simulation center, one might think that vast amount of resources would be needed. The learning from St. Petersburg Research Institute of Emergency Care is that this can be done with minimum resources and some tools provided by the Angels Initiative.
Needless to say, we are extremely proud to be a small part of this movement, which we are certain will shift the landscape of stroke care in Russia and will do everything that we can to continue supporting it!
Watch a video about this simulation center here: https://youtu.be/b4VNwWlRhLk (only available in Russian)