The butterfly is a wonderful creature achieving its beautiful appearance only after passing through several stages of its life cycle. During various stages, the butterfly requires enough nutrients and materials to grow as well as support from the environment. We can observe in some hospitals a very similar “life cycle”. Such an example in improving the quality of stroke care has been found at the Regional Hospital of Příbram in Czech Republic.
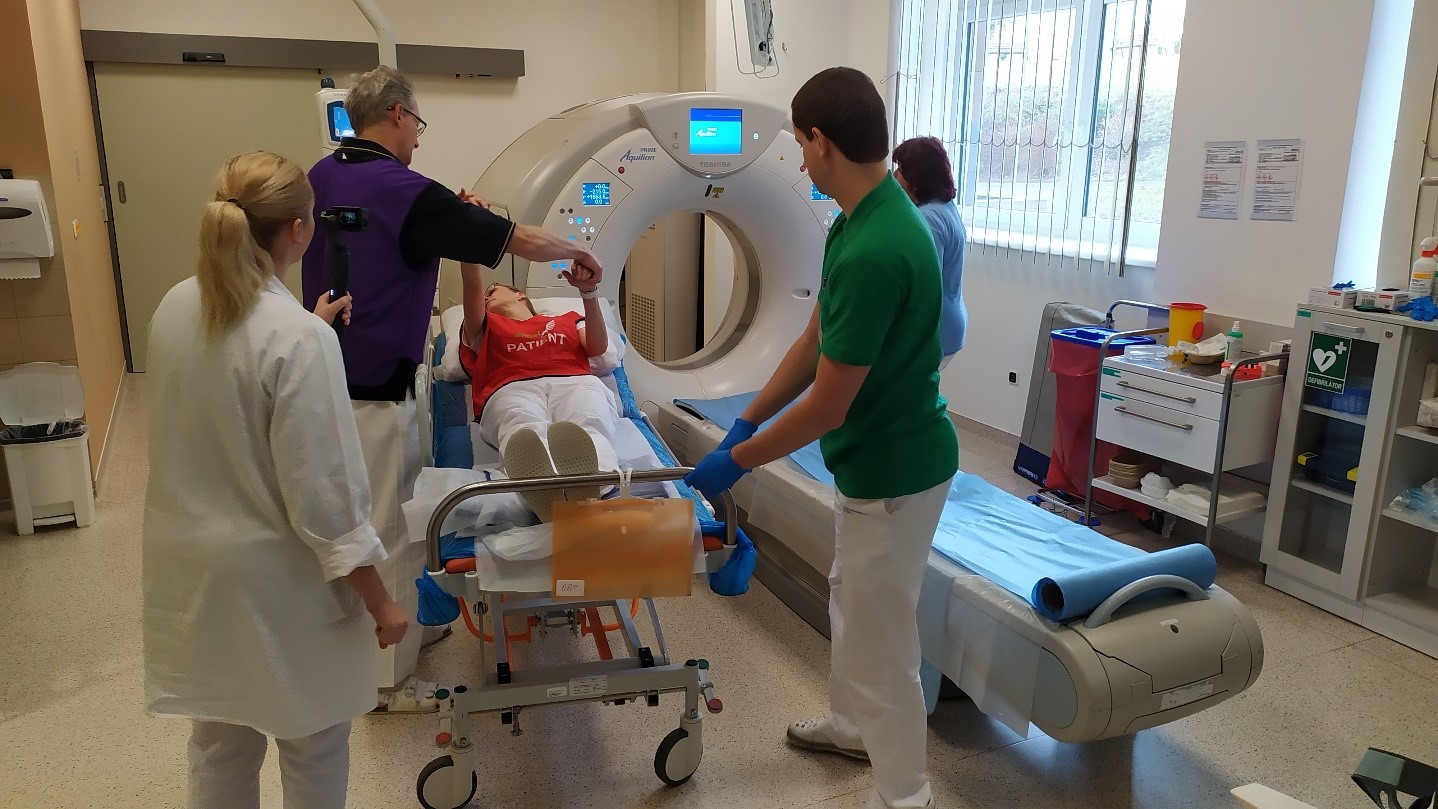
Simulation training with a dummy stroke patient in Hospital Příbram
The story started when the hospital, together with Angels Initiative consultant, performed two rounds of simulation in January 2020 with the goal to improve stroke care for patients. Based on observations from the simulations, the team prepared and introduced an action plan for stroke care improvement to practice step-by-step in the following weeks. Firstly, an optimization of local pre-hospital care appeared to be crucial. Modifications were mostly focused on the needs and content of pre-notification, which consists of information sharing between the neurology department and the EMS professionals before a stroke patient’s arrival at the stroke center.
A multidisciplinary meeting was key in order to define roles for all involved departments: local EMS, ICU, emergency, radiological and neurological department and the hospital management. Since then, the EMS Professionals have been pre-notifying the stroke center accordingly with structured calls containing all relevant information regarding the patients suspected for stroke, which enables the preparation of the entire stroke team and the CT scan before patient arrival. Paramedics accompany the patient directly to the CT immediately upon arrival and remain available for a secondary transport in case the patient is indicated further treatment at larger comprehensive stroke center. These implementations significantly reduce the time required for diagnosis and initiation of therapy. Dr. Jaroslav Machovský, the head of local EMS, acknowledges the cooperation:
“Applied modifications significantly simplified and improved stroke care inside the whole region. Stroke patients benefit the most because EMS professionals are communicating each case directly with the neurologist from the stroke center which increases the quality of pre-hospital care especially in terms of patient’s further direction. Additional but not the least, the effect of EMS and hospital collaboration is a mutual improvement of partnership between paramedics and hospital staff.”
A fundamental change also occurred as for the workload of the Emergency Department Nurses. Nurses are actively contributing to the acute stroke treatment now compared to the mostly administrative role they held before.
Mgr. Lenka Pátková, the head nurse of Emergency department, reacts:
"Based on the recommendations emerging from the simulation training, we have implemented a number of changes during the admission for stroke patients. Currently nurses are well-informed about the time of patient arrival from EMS professionals via the neurologist. Nurses accompany patients directly to the CT as well, where they dilute and administer the treatment. Also, the experience-sharing meeting took place prior to the introduction of the nurse stroke pathway modifications. Mgr. Tereza Koláčná, an experienced head nurse of the comprehensive stroke center at the University Hospital Motol, shared with us working experience with acute and post-acute stroke care of nurses. It was subsequently supplemented by a practical training how properly administer the treatment"

Radiologists now examine stroke patients with the highest priority and play a crucial role in the diagnosis of acute stroke. Currently, treatment administration is enabled inside the CT room immediately after the CT scan. Their presence during an imaging examination can also significantly fasten and specify the streamlines for secondary transport, if needed.
There is a vital piece in the coordination of this entire multidisciplinary stroke team and selection of the treatment. It is based on the right decisions of the Neurologist in charge. Dr. Helena Hlaváčová, Head of the Neurology Department, compares the results of the quality of stroke care:
"We are able to compare data before and after stroke pathway optimization by using the national RES-Q registry reports. While the average time of treatment administration - so called door-to-needle time (DTN), a key indicator of the quality of hospital stroke care, was 60 minutes before stroke pathway optimization. In March 2020, after optimization of the pathway, an average DTN dramatically dropped to 21 minutes. Thus, Hospital Příbram moved from the very last place to a value above average of the entire Czech Republic in just a few weeks".
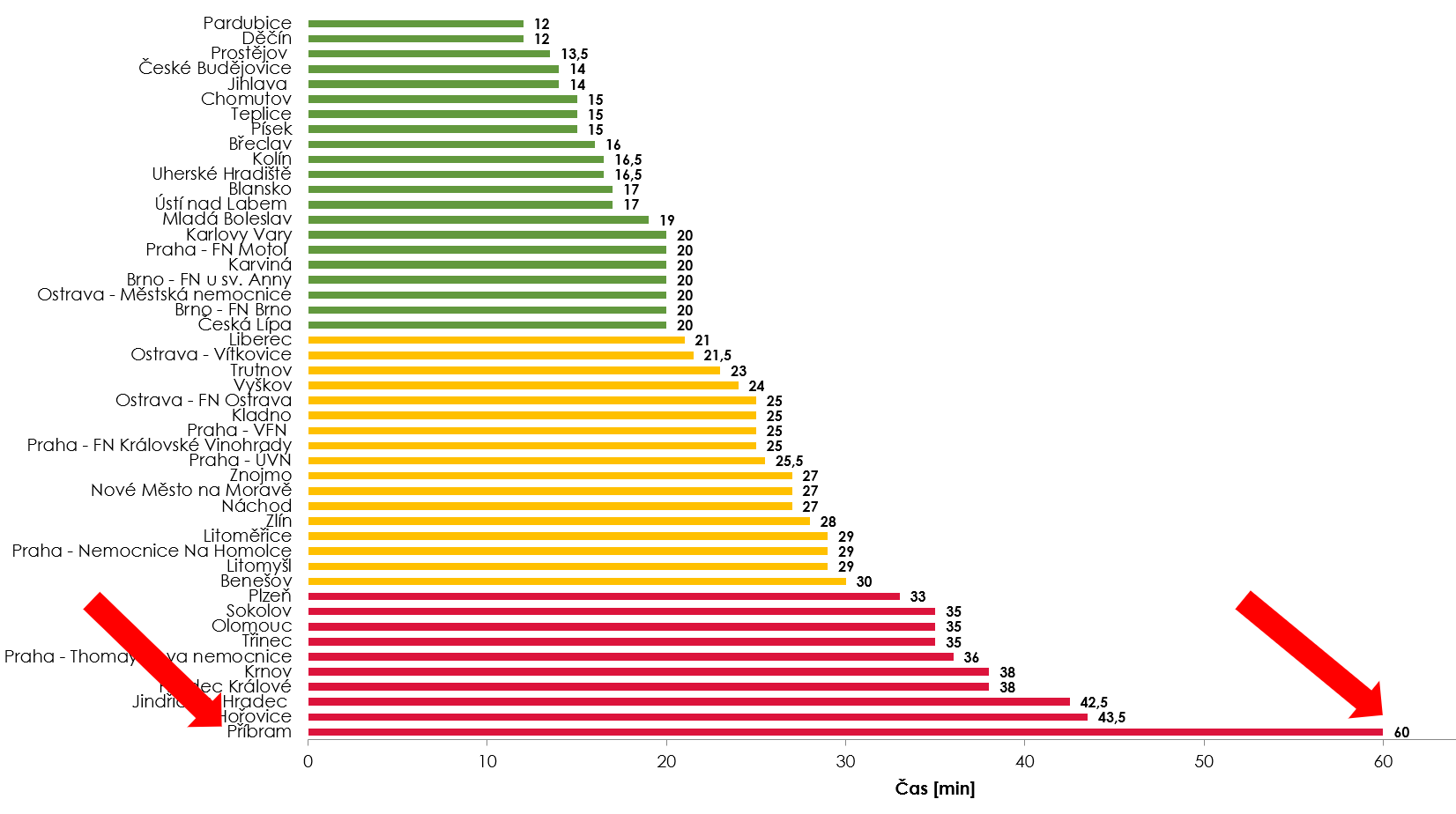
Door-to-needle time (IVT administration) in the national RES-Q report before pathway optimization
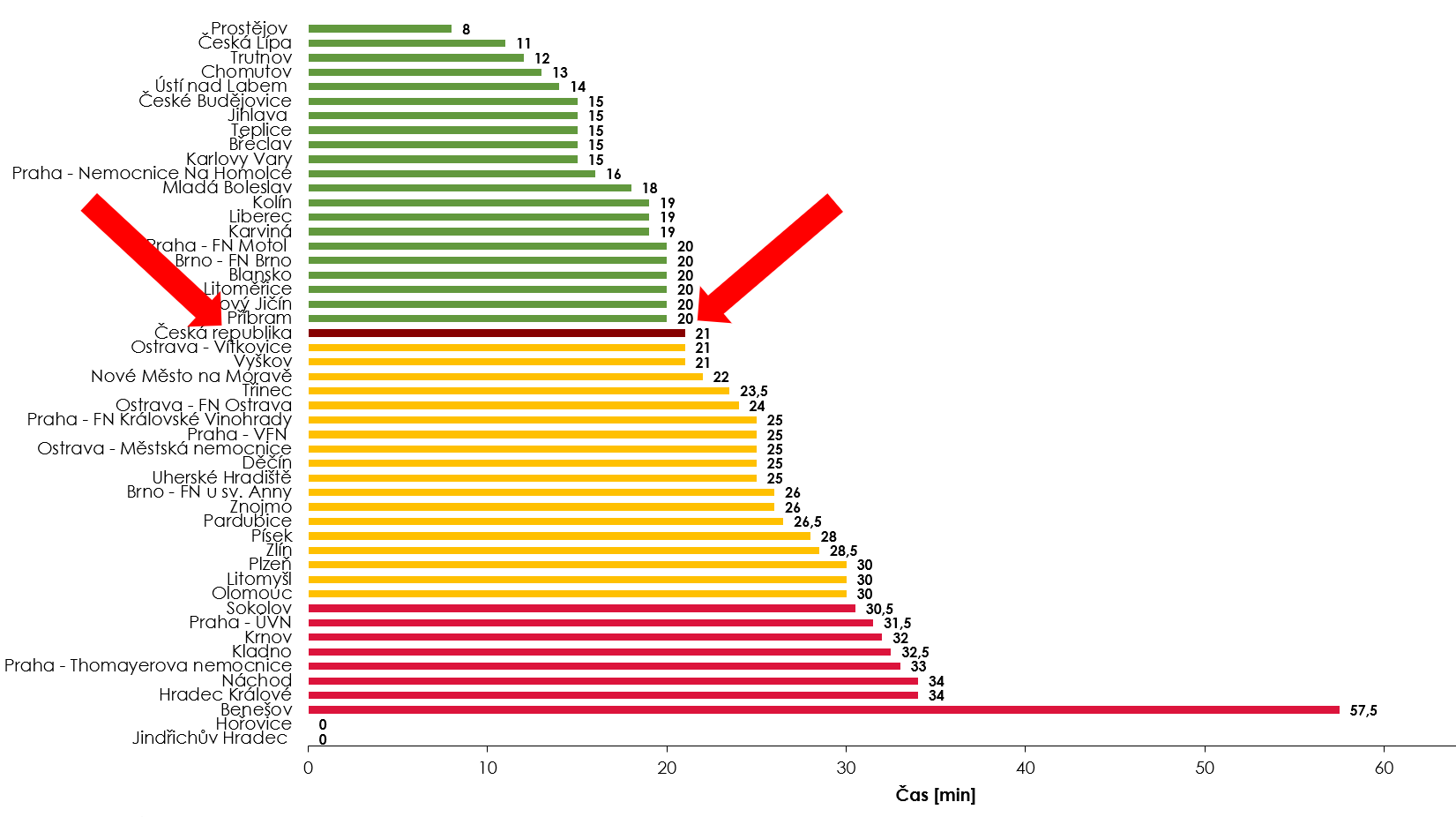
Door-to-needle time (IVT administration) in the national RES-Q report after pathway optimization
The financial costs for such a dramatic improvement are extremely low - just one bedside coagulant-monitor and one automated injector. There were much needed important changes; the change in the existing procedures, in the mindsets of people, and in the desire of all the above to actively participate. We are lucky to be the audience of the gradual development of this exemplary hospital “butterfly” case in the Hospital Příbram where significant improvement in the quality of stroke care was achieved just by desire to change. The change where patients benefit the most.