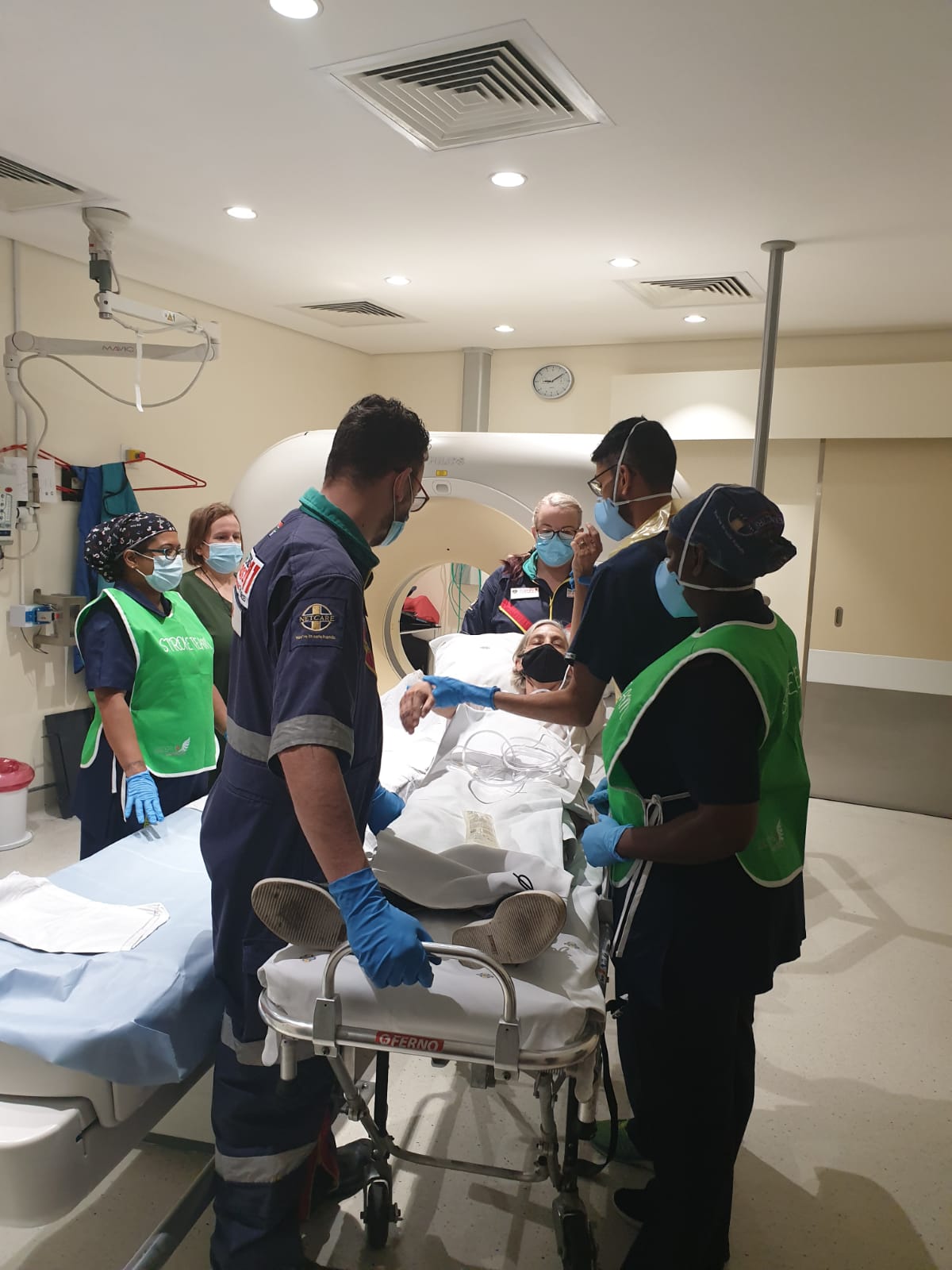
At 8.45am on a sunny Monday morning in Johannesburg, South Africa, an ambulance pulls up outside the Garden Court Milpark, a hotel on the fringe of the city’s central business district. Netcare Milpark Hospital is less than a kilometre away. But the rush-hour traffic slows down progress to the entrance to the hospital’s world-renowned trauma centre where trauma unit manager Sr Zasskia Wiese has been placed on high alert.
The parking lot outside this unit, like those outside hospitals around the world, has seen harrowing scenes play out over the past two years – and at least one of unadulterated joy. In August 2020 frontline workers lined up on the helipad for a dance-off to Master KG’s Jerusalema which had taken a locked-down world by storm.
Before the pandemic, Zasskia would lead her trauma team through a Zumba class on Friday mornings; now they issued a challenge to other hospitals in the region to come out dancing against pandemic burnout. Among those dancing were several of the trauma staff now attending the patient as the two young paramedics wheel the stretcher directly to the CT imaging room.
By the time neurologist Dr Ismail Moola has studied the scans and made the decision to treat by mechanical thrombectomy, the clock on the wall reads 9.22 am. The stroke team at Netcare Milkpark Hospital has once again made good on its reputation for world-class treatment times.
The “patient” meanwhile has suffered no harm beyond losing a button off her blouse, which Zasskia has kept safe. That she is now able to swing her legs off the side of the stretcher and join the team in a review of the morning’s events is no medical miracle – it signals that we have been witnessing a stroke pathway simulation, the first of two that Angels consultant Renathe van der Merwe will conduct this morning.

Zasskia joins the Angels team as they make their way to Steve Biko Academic Hospital, the main teaching hospital of the University of Pretoria, 60 km away. Triage tents are still up outside the emergency departments entrance, testifying to overwhelming pressure on resources at the height of the pandemic. That was also when neurologist Dr Louis Kroon rolled out phase 1 of a stroke care intervention using all the technology and every inch of ingenuity he was able to marshal.
The optimised stroke pathway at Steve Biko now starts at the stroke trolley just inside the emergency entrance where a student has been bundled into a wheelchair to play “patient”. Designed and built by Dr Kroon himself and labeled S-T-R-O-K-E in big die-cut red letters, the trolley is a formidable example of “shaping the path” – an intervention so named by the authors of Switch to describe a strategy for priming an environment for change.
Dr Kroon’s trolley makes it easy to do the right thing in the shortest possible time. Patient information is entered on an iPad (to circumvent the time- consuming administrative process of opening a file) and transmitted to the radiology department and stroke team in real time. The stroke team when summoned will find medication and equipment for examining and treating the patient in easy-to- access compartmentalised drawers. A cellphone app (developed by Dr Kroon with a colleague based in India) connects him to the patient via video and microphone; if a patient arrives outside of his shift, he can direct treatment from wherever he is.

Quite literally shaping the path is a wide green line that starts at the point where the trolley is parked and runs along the mottled grey floor through the hustle and bustle of the emergency department before taking a sharp right turn to radiology. Here, opposite the entrance to the first CT room, the line is broken by the following words: IF STROKE 4.5 H CONT. The meaning is clear. If more than four-and-a-half hours have elapsed since stroke onset, the path continues to the MRI or PET-CT scanner so that decision-making about treatment can be facilitated by perfusion imaging. Dr Kroon’s app also assists with ruling out contra- indications and, once the treatment decision is made, calculates the correct dosage of rTPA according to the patient’s weight.
Because Steve Biko as yet has no dedicated stroke ward (it’s the next project on Dr Kroon’s to-do list, to be followed by making the hospital a thrombectomy- capable stroke centre), stroke patients will spend the next 24 hours in the emergency ward before being assigned to available beds elsewhere. Training is however underway to ensure that nurses in the emergency department understand the importance of the FeSS protocol in post-acute care, and a WhatsApp group alerts the multi-disciplinary team of speech therapist, occupational therapist and physio of a stroke patient in casualty.
The August 2020 dance-off on the helipad was likewise a multi-disciplinary affair, with trauma staff getting into step with physios, dieticians and doctors. Someone brought speakers, the paramedics pulled up in their ambulances; and a trauma surgeon filmed the dance with his drone. Then frontline workers at other hospitals picked up the beat.
After this morning’s events, Zasskia returns to Milpark Hospital thinking about how Dr Kroon’s video-enabled iPad notification system could be replicated at her own hospital. Ideas spread through interactions – and in stroke care as in dancing, a spark is lit when you hear the same music.
* In May 2022, Steve Biko Academic Hospital became the first hospital to receive an Angels Award. Thanks to Dr Louis Kroon's dedication to improved stroke care, the hospital received a diamond award.



